Updated on 5/5/2025
“Mental instability” is a broad phrase people use to refer to a wide range of mental health conditions, from depression and post-traumatic stress disorder to bipolar disorder and borderline personality disorder. When someone uses this phrase, they generally mean that someone is showing signs of mental distress or that their behavior is unpredictable and unstable.
Mental instability isn’t a clinical term or medical diagnosis, and the phrase itself is outdated. Being perceived as “mentally unstable” carries a negative connotation, which can add to someone’s shame or embarrassment over having a mental health condition and make it hard for them to seek treatment. Negative language can stigmatize mental health, so it is a phrase that’s better left in the past.
The Common Symptoms and Causes of Mental Illness
There are approximately 300 mental illnesses and personality disorders recognized in the DSM-5, each with its own set of symptoms and diagnostic criteria. Illnesses can also present differently in different people, meaning two people can have entirely different symptoms but share the same diagnosis. Even so, there’s some overlap with symptoms. Only a mental health care professional can diagnose an illness, but these signs can indicate that someone should seek care.
Common symptoms of mental illness include:
- Aggressive or violent behavior
- Paranoia
- Sleep disturbances
- Confusion or difficulty concentrating
- Social withdrawal
- Suicidal thoughts or self-harm
- Sudden changes in mood
- Persisting feelings of sadness
- Inability to cope with daily problems
- Changes in eating habits
- Physical symptoms such as headaches, stomach pain, or back pain
What Is The Impact Mental Illness Has on Daily Life?
 Mental illnesses and mood disorders can be very disruptive, impacting the individual’s ability to lead a happy, productive life. These illnesses can impact a variety of areas, from interpersonal relationships to performance in class or on the job. Those who don’t seek professional help may try to find coping strategies and self-medicate with recreational drugs or alcohol, compounding the problem and leading to a co-occurring substance use disorder.
Mental illnesses and mood disorders can be very disruptive, impacting the individual’s ability to lead a happy, productive life. These illnesses can impact a variety of areas, from interpersonal relationships to performance in class or on the job. Those who don’t seek professional help may try to find coping strategies and self-medicate with recreational drugs or alcohol, compounding the problem and leading to a co-occurring substance use disorder.
Isolation
Living with a mental health disorder can be exhausting. Keeping up with day-to-day demands, managing stress, working toward personal goals, and maintaining healthy relationships take a tremendous amount of effort and can seem impossible for someone who’s also dealing with an illness such as depression or obsessive-compulsive disorder.
As a result, someone who is suffering from a mental illness may isolate themselves to control unexpected stressors that relationships can bring. The individual may feel as though maintaining relationships requires more effort than they’re able to give, causing them to cut off the people they love. Isolation may also come when someone feels shame over their mental illness or how it’s impacted their life or living environment.
Below-Average Performance at School or Work
School and work both require considerable mental effort and can be tiring for someone without a mental illness. Adding an illness into the mix can make mentally exerting tasks seem impossible. Individuals may have difficulty focusing on tasks, become forgetful, or avoid challenges that feel insurmountable. This can hurt grades and job performance.
Difficulty Completing Tasks
Leaving tasks undone isn’t always a sign of being unreliable or undisciplined. In some cases, it can point to a mental illness. The individual may have racing thoughts that make it hard to see something through to completion, or they may feel too depressed or tired to finish what they started when they weren’t experiencing symptoms.
Neglecting Self-Care
There’s a strong connection between mental health and self-care, and when one is at risk, the other often is as well. Neglecting self-care is often one of the first signs of a mental illness. Depending on the individual, this may mean that they aren’t getting enough sleep, they aren’t taking the time to eat healthy meals at regular intervals, or they aren’t keeping up with their hygiene.
How to Support Someone Who’s Living with a Mental Illness
 In addition to weeding stigmatizing phrases out of their vocabulary, there are plenty of ways someone can provide support to a loved one who’s living with a mental illness.
In addition to weeding stigmatizing phrases out of their vocabulary, there are plenty of ways someone can provide support to a loved one who’s living with a mental illness.
Educate Yourself and Be Open to Talks About Mental Health
Talking about mental health doesn’t come easily to everyone due to persisting stigmas and ingrained ideas about what mental illness looks like. However, education is an effective way to overcome preconceived ideas about what mental illnesses are and who’s at risk of developing them. Being willing to talk to someone experiencing an illness can help empower them to get help or follow their treatment plan.
Avoid Harmful Language and Labels
Remove harmful language, like the phrase “mentally unstable,” from your vocabulary when referring to someone with a mental illness. Such language reinforces negative stereotypes and can further isolate the individual. Empowering, compassionate language can help the affected person feel understood and supported.
Help With Setting Goals
When someone is living with a mental illness, accomplishing tasks such as daily cleaning, personal care, or work-related tasks can feel impossible. Loved ones can support them by helping them set realistic, measurable goals. Meeting these goals can bring a sense of accomplishment and boost confidence.
Don’t Make Assumptions
Don’t assume to know what the individual needs. Ask how you can help, and take time to listen to the response.
Encourage Them to Seek Professional Help
A strong support system is beneficial for everyone, particularly those living with serious mental illnesses; however, this isn’t a substitute for professional treatment. A support system can help someone manage the symptoms of their illness and find coping strategies, but a professional can help them get to the source of the illness and provide a customized treatment plan.
Seeking Professional Help for Mental Illness
 Mental illnesses rarely resolve on their own and can become worse over time. In most cases, people living with mental illnesses benefit from professional help.
Mental illnesses rarely resolve on their own and can become worse over time. In most cases, people living with mental illnesses benefit from professional help.
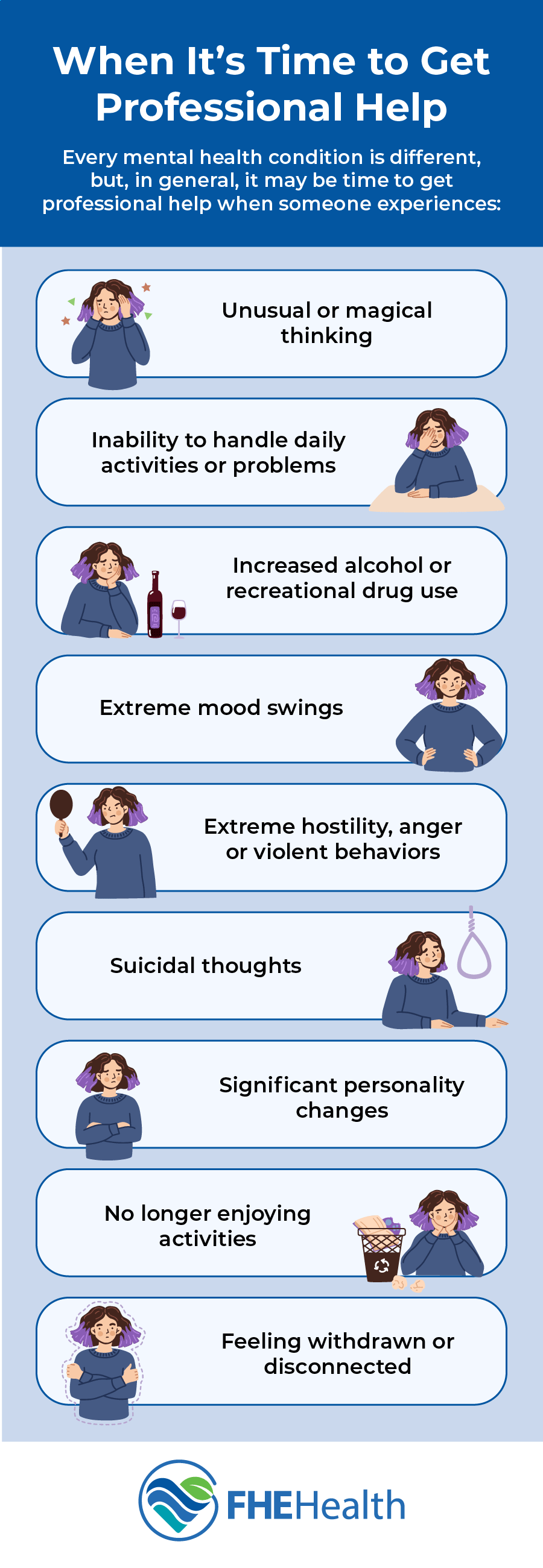
How to Know When It’s Time to Get Professional Help
Every mental health condition is different, and what one person may feel able to cope with may be disruptive for someone else. In general, it may be time to get professional help when someone experiences:
- Unusual or magical thinking
- Inability to handle daily activities or problems
- Increased alcohol or recreational drug use
- Extreme mood swings
- Extreme hostility, anger, or violent behaviors
- Suicidal thoughts
- Significant personality changes
- No longer enjoying activities
- Feeling withdrawn or disconnected
While mental illnesses can cause someone to behave out of character, those living with these illnesses are still responsible for their actions. Getting professional help is one way in which an individual can take responsibility for unacceptable behavior and resolve underlying issues that compromise their relationships or ability to fulfill obligations.
What Kind of Help Do Mental Health Care Professionals Provide?
Mental health care professionals are highly trained and educated to diagnose and treat mental illnesses. Just as treatments vary depending on a physical illness or condition someone may have, mental health treatments differ based on the individual’s concern or condition. Most mental health care professionals provide counseling, either in a one-on-one or group setting. Some are licensed to prescribe medications that may help control symptoms.
How to Find a Mental Health Care Professional
There are several options for finding a mental health care professional, including:
- Getting a referral from your primary healthcare provider
- Getting a list of covered providers from your health insurance company
- Talking to trusted friends, local family members, or clergy
- Determining whether your school or workplace provides mental health services
- Contacting a national health organization such as the National Alliance on Mental Illness
- Conduct an internet search to see providers and client reviews in your area
Before choosing a mental health care provider, pay attention to issues such as:
- Their level of education
- How long they’ve been practicing
- If you intend to use insurance, whether they accept your plan
- Office hours, location, how long the sessions are, and fees
- The areas they specialize in
- Their treatment approach and philosophy
Finding the right match doesn’t always happen immediately, but it’s worth the effort it takes to get effective treatment.
The Importance of Language in Mental Health
It’s important to remember that using terms like “mentally unstable,” even if intended to describe observable behaviors, can be harmful. Such language contributes to the stigma surrounding mental illness and can discourage individuals from seeking the help they need. Instead, focusing on specific behaviors and symptoms and encouraging professional evaluation is a more constructive and compassionate approach. This allows for a more nuanced understanding of an individual’s challenges without resorting to stigmatizing labels.






