
 Alcohol withdrawal symptoms can be intense and even life-threatening. Learn about dependence and how to safely get through detox and recover from addiction.
Alcohol withdrawal symptoms can be intense and even life-threatening. Learn about dependence and how to safely get through detox and recover from addiction.
Recognizing alcohol withdrawal symptoms and understanding their stages is essential to supporting a loved one’s recovery or preparing yourself for the process. Each year, approximately 178,000 people die from alcohol overuse. Many of these individuals have tried to quit but were pulled back due to the intensity of withdrawal. This article provides details about alcohol dependency and the steps most individuals go through during detox and recovery.
How Alcohol Creates Dependency
Not everyone who drinks struggles with withdrawal. A hangover after a night of drinking is different from withdrawal linked to alcohol dependence. Withdrawal generally occurs when a person has developed a dependency.
Dependency occurs when the brain and body adapt to regular alcohol use and begin to rely on it to function. The nature of physical and psychological dependence is intertwined and can’t be wholly separated, but each is worth examining.
Physical Dependency
 The human body is adept at adjusting to its environment. Consider the vastly different diets of a vegan and a sumo wrestler: In each case, the body has adapted to function despite vastly different lifestyles. Similarly, the body can become quite tolerant of regular alcohol use.
The human body is adept at adjusting to its environment. Consider the vastly different diets of a vegan and a sumo wrestler: In each case, the body has adapted to function despite vastly different lifestyles. Similarly, the body can become quite tolerant of regular alcohol use.
After months or years of consuming alcohol, the body expects this external chemical and has actually changed its regulation to accommodate it. It’s possible to develop a physical dependence on just one or two drinks a day, but most addictions stem from long periods of consuming large volumes of alcohol. The sudden cessation of alcohol produces a severe imbalance in the body and a host of side effects. Further complicating the withdrawal process is the abrupt loss of any psychological relief drinking provided.
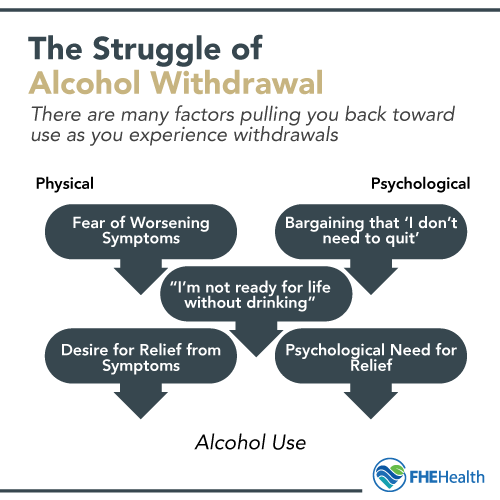
Psychological Dependence
Many people use alcohol to self-medicate. Restricting access to it removes a stress-relief tool that’s become essential for those in active addiction, regardless of its negative physical effects. This increased stress, along with symptoms of physical withdrawal, can be an overwhelming combination.
What Happens During Alcohol Withdrawal?
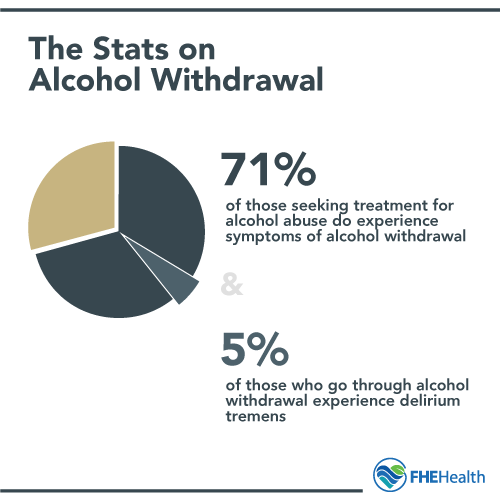
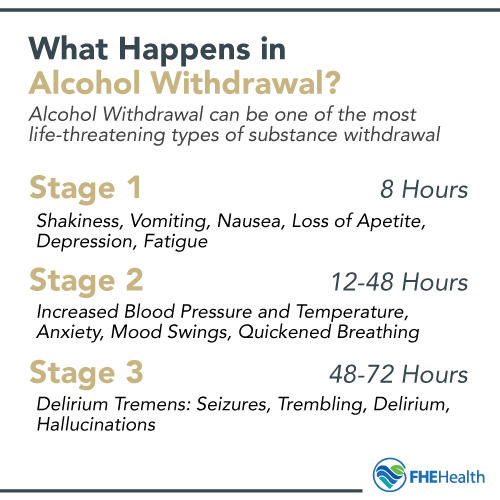 Alcohol withdrawal usually starts within 8 hours after the last drink and can reach its peak between 24 and 48 hours. The way a person reacts during detox depends on their level of use and individual health. However, the entire process typically follows a similar timeline for everyone. It’s estimated as many as 71% of patients seeking treatment for alcohol abuse experience symptoms of alcohol withdrawal.
Alcohol withdrawal usually starts within 8 hours after the last drink and can reach its peak between 24 and 48 hours. The way a person reacts during detox depends on their level of use and individual health. However, the entire process typically follows a similar timeline for everyone. It’s estimated as many as 71% of patients seeking treatment for alcohol abuse experience symptoms of alcohol withdrawal.
Stage 1: Early Withdrawal (6 to 12 Hours)
During the first stages of alcohol withdrawal, a person will feel uncomfortable. They may experience a rapid heartbeat, feelings of nervousness and sweating. Some people have tremors, develop a fever, struggle to sleep and experience changes in blood pressure. This is the body’s immediate reaction to not having alcohol.
During this stage, cravings are strong as the brain encourages the person to drink. This is where having medical support can make all the difference.
Stage 2: Peak Withdrawal (12 to 48 hours)
In peak withdrawal, the pain becomes harder to overlook. The person may also feel a bit more disoriented and confused. It’s hard to focus on what’s happening or what needs to be done. Many experience increased blood pressure, temperature and mood swings.
Hand tremors are common. Some people may also develop seizures. The person shouldn’t be alone during this time or going forward.
Severe Withdrawal (48 to 72+ hours)
During this time, the body is experiencing the full effects of functioning without alcohol. Operating without alcohol means the body is still overcompensating and reacting to reality without the substance. The body reacts to the symptoms, meaning blood pressure, heart rate and nervous system are all heightened. A person may experience an alcohol withdrawal seizure, nausea and fatigue.
A Medical Emergency: Delirium Tremens
Delirium tremens is a severe condition that 5% of those with dependence will experience. It includes hallucinations and severe seizures. Any patient who experiences delirium tremens needs immediate medical attention, as the condition is life-threatening.
The Importance of Medical Detox
Attempting alcohol detox at home can be dangerous and painful. Without medical and emotional support, home detoxes are often unsuccessful, as well as potentially life-threatening.
However, in an alcohol detox facility, the process is much safer and often more effective.
The benefits of medical detox include:
- Around-the-clock monitoring. In medical detox, professionals are available to monitor vital signs and respond immediately to complications.
- Symptom management. Individuals may be prescribed medications and therapies to manage withdrawal effectively. IV fluids may be administered to prevent dehydration. Anti-seizure medications can be used to prevent harm and manage severe symptoms.
- Safety and support. Detoxing in a secure environment helps prevent relapses and reduce the mental needs associated with withdrawal.
Counteracting Alcohol Withdrawal Symptoms: When to Get Help
It’s not easy to manage these situations on your own. You may try to sleep through it, but it’s unlikely you can because your body is going through a sometimes-violent experience in reaction to the withdrawal. It’s better to be in a medical facility where your care can be monitored and any life-threatening risks can be removed or controlled.
Frequently Asked Questions
Getting Help for Alcohol Addiction
If you or someone you love is struggling with alcohol addiction or experiencing alcohol withdrawal symptoms, you’re not alone. Contact FHE Health to learn more about your treatment options.






